Table of Contents
Meet Dave Heath – Former Ambulance Paramedic, turned Oncology and Urology Nurse Practitioner (NP) at Bendigo Health and Goldfields Urology. He is also the first nurse in Australia that performs prostate biopsy.
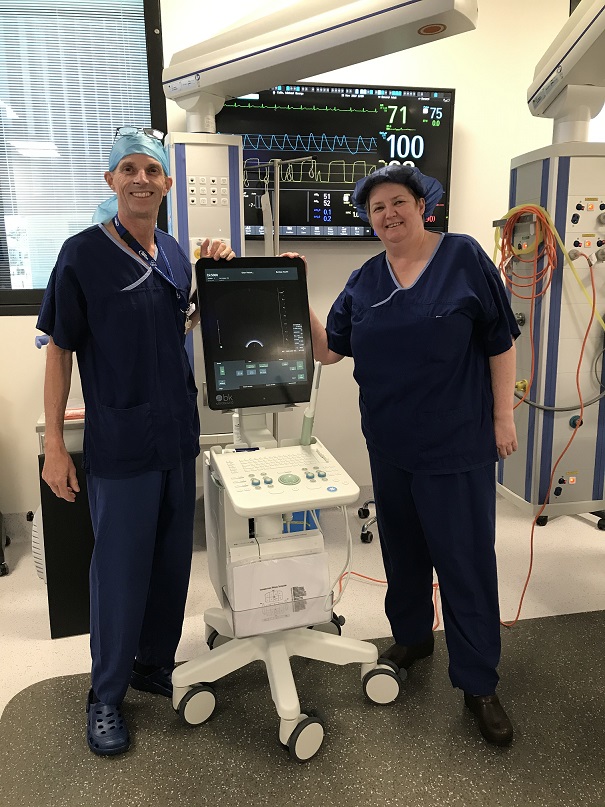
You started your career as an Enrolled Nurse, can you tell us a bit about that time?
I started as an EN in the late 90s as a mature age TAFE student. Previously I had been in the building trade as a Painter and Decorator from a teenager. It was time for me to change my working life as I had begun to experience some minor physical complaints from the physically of the building trade and figured that this would be exacerbated with age. The EN course provided me with an opportunity to dip my toe into nursing and would eventually provide me with a great base to expand on.
In 2012, when you became a prostate nurse it was a pilot program, can you tell us a little more about the role and how it looks now in 2020?
I was fortunate enough to hear about a proposal for a specialist nursing role that focused on the care of men with prostate cancer. I first heard of this proposal in 2010 and decided that I should look into the course that was offered and undertook some “more study” (distant). Upon completion of this post-grad course, I then heard the exciting news that Bendigo had been awarded one the 3-year pilot positions funded through both the Prostate Cancer Foundation (PCFA) and Movember (I had previously grown a number of dodgy-looking moustaches in my time).
When the first 12 positions were advertised nationally I was interviewed for the Bendigo position which started as a part-time 0.7 role and was again fortunate enough to be successful in being involved in this initial pilot program. Ambulance Victoria was supportive of me reducing my EFT to a part-time paramedic which allowed me to continue in both roles for the first 12 months.
The role of Prostate Cancer Specialist Nurse (PCSN) I’m proud to say has cemented itself nationally and grown to the point of 80 current positions with 95 positions by the end of 2021. I remain affiliated with the PCFA despite no longer holding the title of PCSN which enables me fantastic networking opportunities along with financial assistance with professional development opportunities.
The PCFA financial assistance that I am entitled to has directly supported progression to my current role as it enabled me to visit the UK for procedural training and international meetings which has enabled me to be endorsed as the first nurse in this country that performs prostate biopsy.

You are currently working as a Oncology and Urology Nurse Practitioner . What does a typical day look like?
My job has grown to include not only prostate cancer but also bladder and renal cancers. These additional cancers have their own investigations and follow-ups. From a clinic point, I am involved in all the consultant outpatient clinics where I see both new referrals and review patients. These patients I manage independently but as always I have the medical staff for anything that I am unsure about or out of my scope.
I also have a weekly NP led clinic that consists of urological oncology follow up patients. This group consists of prostate, bladder and renal cell predominately (occasional testicular cancer). This clinic I run with the help of the junior medical staff and urology trainee positions which includes the registrar and fellow.
I supervise the outpatient trial of voids, attend the wards for difficult catheter insertions. I do the referrals for radiotherapy and pre-operative pelvic floor education.
I have 3 theatre lists per month which consist of flexible cystoscopy lists for follow up of bladder cancers and investigation of haematuria. Plus I also have the prostate biopsy list that includes the biopsy but also placement of fiducial markers (gold seeds) for men having radiotherapy for prostate cancer.
A normal day starts at 0700 with checking emails/messages then sometimes I go on the ward round (depending on which patients are in) after the ward round if I have a list that day I head off to theatre and if I don’t have a list I will go to the clinic. The times I’m not in the clinic or have a list, I do my admin and really whatever pops up as it only takes a phone call for the day to change. I also work privately in consulting rooms which also forms part of my 4 weekly rotating roster.
What are some of the common clinical presentations you see?
Prostate Issues
I see new referrals for elevated PSA (prostate blood test).
These can also have bladder symptoms i.e. difficulty with passing urine.
The first appointment
Consists of me taking a history including co-morbidities, medications, and allergies, presenting complaint/ symptoms (if any as an elevated PSA in isolation can be symptom-free), family history, smoking status, home environment and employment.
The next part consists of an examination
I always take time to discuss indication for examinations as I feel strongly if the patient is of the same understanding as to why the examination forms a large part they are more relaxed and confident in my management moving forward.
The examination consists of a lower urinary tract exam in that I access for a palpable bladder, I access for flank tenderness, I exam external genitalia and perform a digital rectal exam. For a patient with a high PSA and or other symptoms suggestive of advanced disease risk I will perform a neuro exam plus general thoracic and cervical skeletal exam (? Bone disease and symptoms suggestive of bone pain).
Investigations
Investigations for elevated PSA referrals consist of imaging with CT, Ultrasound, Bone scans (depending on presentation) and MRI which requires a consultant to request as does a Pet scan. Pathology and urine tests are something that I routinely request, pathology consists of repeating the PSA, renal function and occasionally LFTs (again determined on a case by case basis). These investigations are then reviewed and assist in guiding both management but also a response to any treatments that may have commenced.
Some of the treatments used include medications for bladder symptoms, these medications are most commonly ALPHA blockers which help relax the bladder neck and can at times improve obstructive symptoms.
Prostate Biopsy
For a man with a persistently elevated PSA (each man is accessed independently despite PSA ref range) i.e. a PSA that is not appropriate for that man and his prostate (it’s a size thing) is commonly a biopsy of his prostate.
A prostate biopsy is a procedure that comes under my scope of practice as a NP they then end up on one of my lists for the biopsy. Post biopsy they are then followed up in the NP outpatient’s clinic that I run with regards to results and discussion around next step (depending on results).
Erectile Dysfunction (ED)
I See men with erectile dysfunction (ED).
These consults again involve a thorough history taking and also a physical examination. Pathology investigations including a cardiovascular screen as declining erections can be an early sign of cardiovascular disease.
Imaging mostly consists of ultrasound for men with reported Peyronie’s disease (I have been trained in corporal ultrasound and we are able to offer this in the private rooms).
TNB addition: ‘Peyronie’s disease is a connective tissue disorder involving the growth of fibrous plaques in the soft tissue of the penis. Specifically, scar tissue forms causing pain, abnormal curvature, erectile dysfunction, indentation, loss of girth and shortening.’
The management for erectile dysfunction (ED) in the first instance is mostly pharmacological i.e. drugs, but in saying that surgery also plays a role for some men with ED and some forms of Peyronie’s this is obviously not something that I perform but I am involved in both the pre-op and post-op care/ management and follow up.
Bladder Cancer
Bladder cancer is another urological condition that comes under my scope.
Flexible cystoscopy
My involvement with bladder cancer patients consists of surveillance flexible cystoscopy, this procedure is done as a day case and involves the use of a scope that provides an image of the lower urinary tract. The purpose of cystoscopy surveillance is to inspect and examine for bladder cancers. Pre-op investigations include pathology (predominately UEC) urine analysis for infection and malignant cells, imaging in the form of either a CT or Ultrasound depending on presentation.
Another part of my role in bladder cancer follow up is for patients that have undergone a cystectomy with either a neobladder or conduit. The long term follow up and monitoring of these patients form an increasing part of my role.
Renal Cancer
Finally, renal cancer patients come under my care in regards to long term follow up and monitoring.
These patients have routine imaging and pathology investigations for 5 years and are a patient that I see in my outpatient clinic. The imaging consists of CT and Ultrasound (depending on the individual case) and pathology is routine full blood exam and renal function.
What are some of the biggest challenges of working as an oncology and urology nurse?
Some of the bigger challenges include workload (as is the case for all of us) plus being able to separate work from home. There is always at least one patient that occupies some of my thoughts when I’m not actually at work but I am ok with this as I feel it comes with the territory.
I am very aware that my role is a privileged one in that I see patients that are dealing with one of the biggest challenges they will ever face and I actually am fortunate in that these patients have taught me a great deal in how to face such huge challenges.
What are some common misconceptions about your field?
I guess the biggest one is that we are always seeing patients with a poor prognosis and that they have a terminal illness. This couldn’t further from the truth in Urological Oncology whilst we still do see patients with advanced disease the majority of our patients have treatable / manageable disease and as such this forms a large part of my role in the long term monitoring of these patients.
Why should more nurses consider urology nursing as an area of clinical interest?
Urological nursing in my opinion provides nurses with an opportunity to specialise to the point that they are able to significantly contribute to a patient’s management. This management can be both during inpatient admissions but also outpatient followup and reviews. Urology nursing provides a great deal of autonomy for nurses (not just NPs) in that a large amount of the post-surgical management is something that a suitably qualified nurse can lead and manage on the wards and outpatient clinics.
From my point of view, it has provided me with the opportunity to expand my scope as an NP to the point that I am the first urological nurse to be performing prostate biopsy procedures in Australia (to my knowledge). Nurse-led biopsy has been in place in the UK for a number of years but not in Australia until now.
Can you tell us a little about working with Prostate Cancer Foundation Australia (PCFA)?
As I mentioned earlier the role of PCSN was commenced in 2012 with a joint project between the PCFA and Movember. The PCFA is a leading organisation that provides information and support through research and obviously specialised nursing roles for men and their loved ones with prostate cancer.
What is the men’s BBQ?
The annual Big Aussie Barbie (BBQ) has been run for greater than 10 years and has made a significant contribution in regards to both raisings of funds that support research and other PCFA activities but also the opportunity for men to gather and network. This networking creates an opportunity for discussion around prostate cancer diagnosis/ management and overall men’s health on a whole.
I became involved in the early days with a local event that was organised to create awareness around men’s health issues including prostate health. I and another Nurse Practitioner attended and gave a short informal presentation of which mine focused on prostate health / awareness.
What is the most important piece of advice you can give men about prostate health?
For me, the most valuable piece of advice/ information around prostate health is to be aware of your own family history in regards to prostate issues (not just cancer) and to have a good understanding of your own PSA result. It’s important to be aware that PSA is a variable test that differs greatly between men and that not all men and their PSAs are the same.
Like all body systems, there are times when a specialist needs to be consulted and the prostate is no different. If a man has an increasing PSA and or symptoms he should be referred for a specialist opinion to evaluate that individual’s symptoms and risk. It’s important to ensure that men are informed off all the things that increase a PSA and that’s it’s not a cancer test specifically it’s more of a size/ inflammation test and each case needs to be evaluated on its own merits by a suitably qualified clinician.
How can our readers within the healthcare community best contribute to men’s health and wellbeing?
In my opinion, the best way to contribute to men’s health is to ensure that we all create the opportunity for conversations. This is not always an easy thing but with enough time and an environment that allows for conversations to take place, it can be amazing the topics that come up.
Are there any resources you would recommend for the readers that could help raise awareness around men’s health and wellbeing?
There are obviously thousands of resources available especially within the world of internet and the access that we all have within the palm of our hands. The only advice that I give to be wary of anything that either sounds too good to be true or involves a cost.
If you could turn back time, what advice would you give your younger self?
The only advice I would give myself is the thing that comes with maturity in that we should all back ourselves not only professionally but also privately. If you put the work in you will see the rewards (however that looks for the individual).
Do you have any advice for Registered Nurses who are interested in becoming Nurse Practitioners?
For any registered nurse that identify a clinical speciality that they are passionate about and feel that they could perform their role within that speciality better with an increased scope definitely NP is the way to go. Don’t be put off by the perceived workload as is the case with all things if you apply yourself you will achieve the goal.
Do you have one person who has been influential to you and why?
I actually don’t have a single person that has influenced me but in saying that there have been multiple people/ clinicians and patients that have inspired and amazed me over the years. The resilient nature of humans is amazing and continues to surprise and motivate me.
If nothing else 2020 has definitely shown how adaptable we all are not just within the health profession.
Check out our other nurse practitioner related articles
Check out our other oncology nursing related articles
Looking for our next guest! Are you / do you know of a healthcare worker or student working in Australia, who would like to write about your/thier career, area of speciality, unique experiences or other nursing/midwifery/allied health related content? Please email us at hello@thenursebreak.org to discuss further or check out the Write for TNB Info Page on the website.






You must be logged in to post a comment.